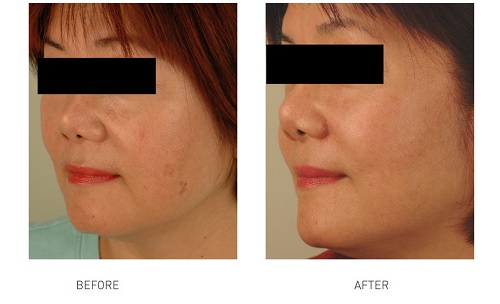
It is a common skin disorder resulting in brown to gray-brown patches, and commonly appears on the face, especially on the cheeks, forehead, chin and the bridge of the nose. Because melasma is so common and has a very characteristic appearance the diagnosis of melasma is made by the physician in most cases by just looking at the skin.
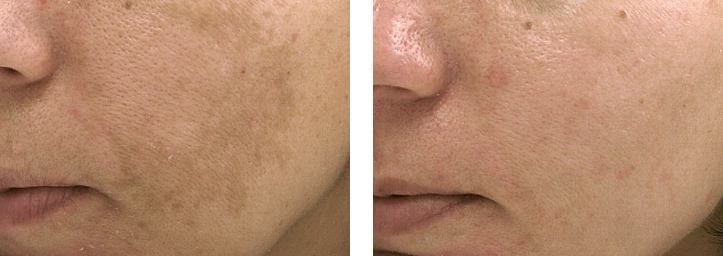
Melasma is typically grouped into three large categories based on the depth of melanin pigments; epidermal melasma (pigments in superficial layers), dermal melasma (pigments in deep layers), and mixed type (pigments in both superficial and deep layers), but this classification is based on a flawed study that was conducted more than two decades ago. Clinically more relevant classification should be based on known histological changes (microscopic changes within the skin).
The cause of melasma is believed to be due to an increase in the production of cells which release the pigment melanin, resulting in darkening of the skin. Commonly known as the mask of pregnancy, chloasma is melasma acquired during pregnancy.
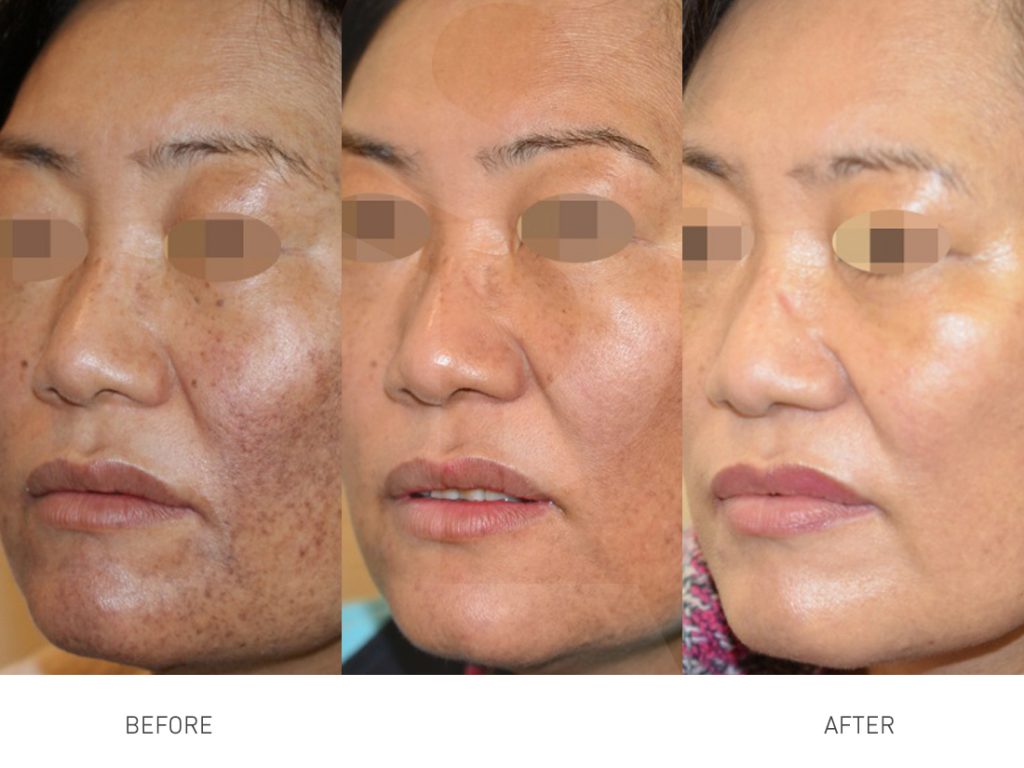
There are multiple factors which are thought to trigger melasma including some cosmetics, birth control pills, hormone therapy, drugs that cause sun sensitivity, certain antiseizure medications, sun exposure. Although some melasma may disappear spontaneously after menopause, melasma generally does not regress on its own and is one of the most resistant pigmentations to treat.
Most cases occurs in women; however, 10% of cases affect men. The condition is universal and seen in all cultures and ethnicities; however, it is far more commonly seen in people with darker skin tones including those of Asian, Hispanic, Latin, Indian, Middle Eastern, Mediterranean and North African descent.
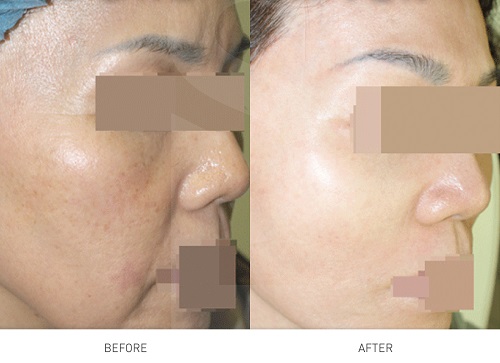
Individuals with these backgrounds have higher levels of melanin in their skin and a tendency to tan. There often is a family history of melasma. Individuals with fair skin may experience a lighter shade of melasma which is not always recognized.